Seborrhoea
Pääsivu:Ihoaiheet
article.category:Skin Diseases
Seborrhoea is essentially taken to mean the over-production of oils by the sebaceous glands in the skin. Seborrhoea is a symptom that conveys no information on the underlying cause. It appears as an associated manifestation of seborrhoeic eczema (also called seborrhoeic dermatitis).
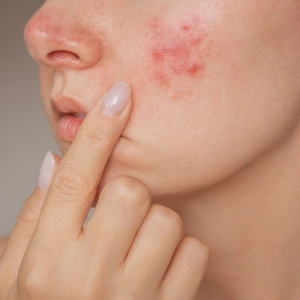
Cause
Seborrhoeic eczema takes a chronic course involving relapses and affects approximately 1% to 5% of the population. It preferentially affects areas of skin with high numbers of sebaceous glands, such as the scalp, forehead, nose, nasolabial fold, eyelids, the back of the neck and the axilla. Those affected suffer from whitish to yellowish, usually oily, shiny scales. The skin is reddened below these scales. Severe itching may also occur if the scalp is affected. Seborrhoeic eczema is far more common in men than in women, especially between the ages of 18 and 40. We do not know exactly how it develops. The fungus Malassezia furfur is viewed as a potential trigger. Several factors can favour the development of seborrhoeic eczema or exacerbate its symptoms, including hormone levels, specific genetic predisposition, a weakened immune system, climate, stress and lack of sleep.
Options for treatment
Seborrhoeic eczema is mainly treated topically. The aim is to remove the symptoms or at least to alleviate them. To this end, local antifungal drugs (antimycotics) are used in shampoos or ointments. Most of these products also have anti-inflammatory properties and thus soothe irritated areas of the skin. The temporary use of cortisone may be useful in severe forms.


